You’ve sold the vision. By becoming a self-service, data-driven healthcare system, you will improve the bottom line and make your hospital system more competitive. You’ll improve the quality of care for every patient, and allow the organization to blow the doors off your patient satisfaction scores by tailoring services to predict the patient’s ideal meal selection along with the best possible care outcome. You’ve purchased and deployed the latest data warehousing appliances and data management suite. You’ve spent months integrating data from the far corners of your enterprise. You’ve selected the sexiest self-service business intelligence tools on the market. You’ve trained thousands of users, stood up centers of excellence, presented your pilot program results to physician leadership and executive management. Your healthcare analytics program is live and medical miracles are waiting to reveal themselves out of your data. Or maybe not.
The healthcare analytics market for 2016 is expected to top $9.96 billion USD with a +26% compounded annual growth rate (CAGR) over the next 5 years, reaching almost $32 billion annually in 2021. Sixty-one percent of that investment, or more than $6 billion this year, is coming from the North America healthcare. In comparison, the juggernaut US EMR/EHR market was only a third larger at $9.3 billion in 2015 with a far more modest 7.1% annual growth rate.
Yet, despite the massive investment and some very promising anecdotes, wide spread use and adoption of analytics, especially self-service BI, feels like it is falling short of the vision and potential value. While quantifying the value of analytics efforts is notoriously challenging, only a few of the healthcare organizations I’ve spoken with will tell you they are getting everything they need and expect out of their analytics platforms and investments.
Let’s look at some of the remaining challenges standing in the way of fully realizing the value of an analytics investment and see if there might be some common root causes that we can address.
- Integrating the Data is Difficult/Resource Intensive: Even with widespread adoption of Big Data technologies and techniques to make “landing the data easy,” organizations still require a significant amount of real data integration work to semantically and coherently bring complex healthcare data together from across the myriad of systems, applications, and data warehouses residing inside and outside of walls of your organization. Effective use of data requires understanding the “data map” of its journey and relationship to other complementary or contradictory data.
- Differences Extend Beyond the Data: Before we can have our data semantically normalized, we have to address differences in our semantics across the organization. We’re still sorting out how to communicate with other ancillary care departments, so it shouldn’t be surprising that there are differences in how clinical care, billing, and the new health plan communicate when acting as an enterprise. These differences range from how we define a “length of stay” to how we organize resources within our various divisions or facilities. Variation makes analysis – and analytics – exponentially more complex. We have to be precise in the language we use, thorough in our definitions, and comprehensive in the context provided with all of our analytics solutions.
- Our Data is Messy: We all know healthcare data is complex and often fraught with quality issues. The complexities of different clinical terminologies (ICD-10, SNOMED, LOINC, CPT) make simple things like defining patients with a stroke-related diagnoses labor intensive and error prone. Even when tools are used to profile data in order to assess data quality, results are often abstract and disconnected from how that data is used in a report or analysis. In fact, many self-service analytics users are left without any real gauge of the quality of data they might want to incorporate into their analysis. Users are becoming sophisticated enough to understand that not all data is of the same quality. And, smart users are unlikely to rely on data of unknown quality.
- Now where did we put that…: Many healthcare organizations are, in many ways, suffering an embarrassment of information riches. Virtually all of the EMR/EHR, ERP, CRM, time reporting applications, and hundreds of other systems across your enterprise provide package analytics. This proliferation of tools, along with your custom analytics and data warehouse solutions, means the challenge has shifted from “how do I get the data?” to “where do I find the right data in this mountain of reports?” Unfortunately, too many organizations are still hoping to build their way out of this problem. And they believe they can do just that, if they build enough reports and dashboards. The reality is that this strategy only treats the symptom and actually exacerbates the underlying problem of users not being able to find needed information by adding more data to the heap.
- Data is Still More Important than a Slick Analytics Tool: As easy to use and powerful as today’s leading analytics tools have become, users must still have a basic understanding of data in order to apply the tool in new ways to unlock insights. An outpatient physical therapy manager can’t adapt the Inpatient Physical Therapy Progress Report to her ambulatory needs if she doesn’t know where to find the outpatient physical therapy case report data.
While the above list of challenges facing healthcare data governance programs is not exhaustive, these common analytics adoption challenges identify a pattern of poor data governance as a significant contributing issue. The root causes include:
- Lack of data lineage
- Poorly defined business terms
- Ill-managed clinical vocabularies/terminologies
- Inadequate understanding of data quality
- Lack of consistent, searchable report metadata to make finding the right information possible
To put it plainly, in order to improve the value from analytics investments, we need to focus on data governance. The diagram below represents the concept visual. I encourage you to take an honest look at the value the organization is realizing from your healthcare analytics program today and determine how large the opportunity is to improve the value.
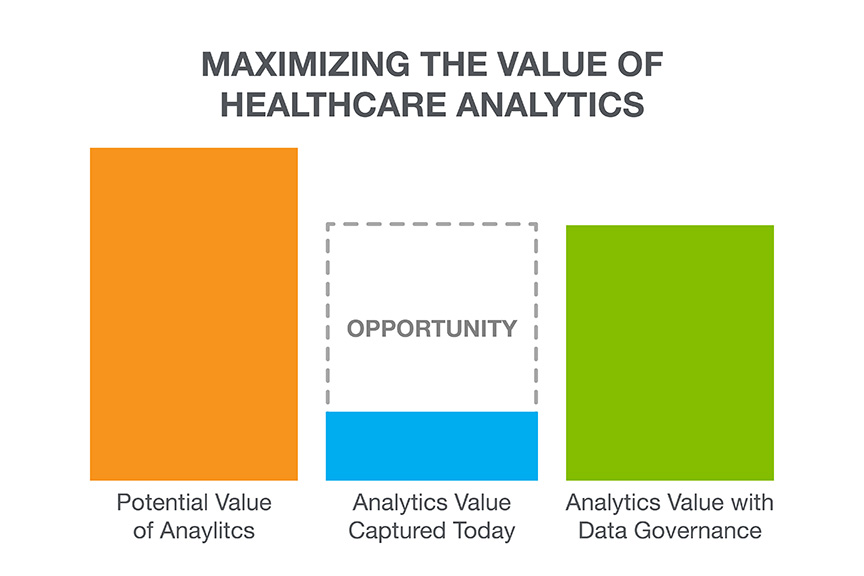
The first step in any self-improvement effort is understanding that improvement is needed. In future posts, I’ll share how and where to focus your data governance efforts to increase the value from your analytics initiatives.




